This website uses cookies so that we can provide you with the best user experience possible. Cookie information is stored in your browser and performs functions such as recognising you when you return to our website and helping our team to understand which sections of the website you find most interesting and useful.
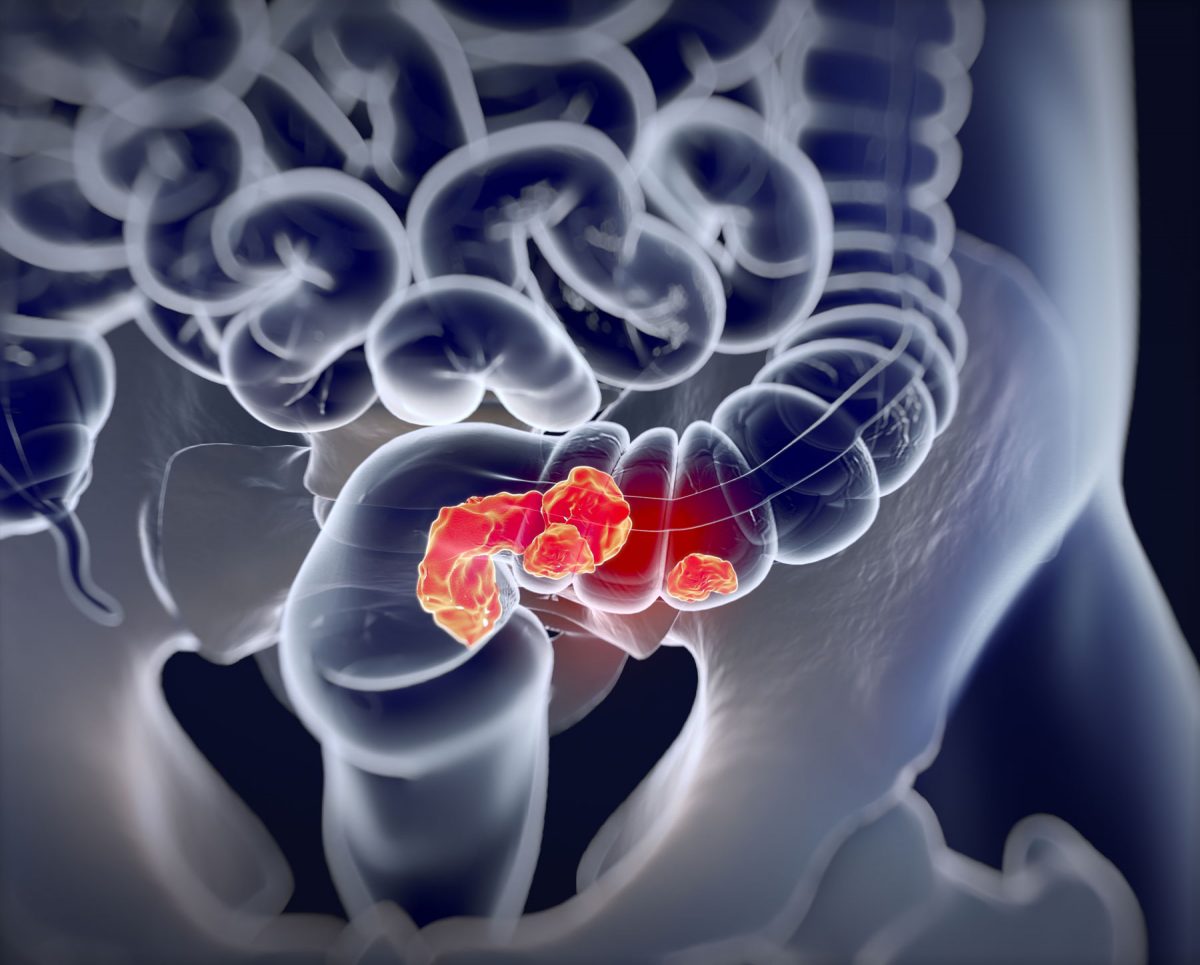
Colorectal Cancer
Colorectal cancer, also known as bowel cancer, colon cancer, or rectal cancer, is any cancer that affects the colon and the rectum.
The American Cancer Society estimate that about 1 in 21 men and 1 in 23 women in the United States will develop colorectal cancer during their lifetime.
It is the second leading cause of cancer death in women, and the third for men. However, due to advances in screening techniques and improvements in treatments, the death rate from colorectal cancer has been falling.
Colorectal cancer may be benign, or non-cancerous, or malignant. A malignant cancer can spread to other parts of the body and damage them.
How does colorectal cancer start?
Polyps in the colon or rectum
Most colorectal cancers start as a growth on the inner lining of the colon or rectum. These growths are called polyps.
Some types of polyps can change into cancer over time (usually many years), but not all polyps become cancer. The chance of a polyp changing into cancer depends on the type of polyp it is. The 2 main types of polyps are:
⦁ Adenomatous polyps (adenomas):
These polyps sometimes change into cancer. Because of this, adenomas are called a pre-cancerous condition.
⦁ Hyperplastic polyps and inflammatory polyps:
These polyps are more common, but in general they are not pre-cancerous.
How colorectal cancer spreads?
If cancer forms in a polyp, it can grow into the wall of the colon or rectum over time. The wall of the colon and rectum is made up of many layers. Colorectal cancer starts in the innermost layer (the mucosa) and can grow outward through some or all of the other layers.
When cancer cells are in the wall, they can grow into blood vessels or lymph vessels (tiny channels that carry away waste and fluid). From there, they can travel to nearby lymph nodes or to distant parts of the body.
The stage (extent of spread) of a colorectal cancer depends on how deeply it grows into the wall and if it has spread outside the colon or rectum.
Where does colorectal cancer grow?
To understand colorectal cancer, it helps to understand the parts that make up the colon and rectum. The colon and rectum make up the large intestine (or large bowel), which is part of the digestive system, also called the gastrointestinal (GI) system (see illustration below).
Most of the large intestine is made up of the colon, a muscular tube about 5 feet long. The parts of the colon are named by which way the food is traveling through them.
- The first section is called the ascending colon. It starts with a pouch called the cecum, where undigested food comes in from the small intestine. It extends upward on the right side of the abdomen (belly).
- The second section is called the transverse colon. It goes across the body from the right to the left side.
- The third section is called the descending colon because it descends (travels down) on the left side.
- The fourth section is called the sigmoid colon because of its “S” shape. The sigmoid colon joins the rectum, which connects to the anus.
The ascending and transverse sections together are called the proximal colon. The descending and sigmoid colon are called the distal colon.
Types of cancer in the colon and rectum
Adenocarcinomas make up about 96% of colorectal cancers. These cancers start in cells that make mucus to lubricate the inside of the colon and rectum. When doctors talk about colorectal cancer, they're almost always talking about this type. Some sub-types of adenocarcinoma, such as signet ring and mucinous, may have a worse prognosis (outlook).
Other, much less common types of tumors can start in the colon and rectum, too. These include:
- Carcinoid tumors
- Gastrointestinal stromal tumors (GISTs)
- Lymphomas
- Sarcomas
Early detection
Doctors are looking for better ways to find colorectal cancer early by studying new types of screening tests (like blood tests) and improving the ones already being used. Researchers are also trying to figure out if there's any test or screening plan that clearly works best.
Diagnosis
Researchers are trying to define colorectal cancer sub-types. This means grouping colorectal cancers based on things like the genetic mutations in the cancer cells, how the cells look and behave, how fast the cells are dividing, and features of the tumor itself.
Lab tests to help plan treatment
Lab tests have been developed to help predict which patients have a higher risk of colorectal cancer recurrence (the cancer coming back after treatment). These tests look at different genes inside the person's colorectal cancer cells. These tests are being studied to see if they might help decide which treatment plan is best for each person. They might also be helpful in deciding if more treatment is needed before and after surgery.
Treatment
Researchers are always looking for better ways to treat colorectal cancer.
Surgery
Surgeons continue to improve the operations used for colorectal cancers. Researchers are looking at the benefits of laparoscopic and robotic surgeries compared to open surgeries (where bigger cuts are made in the skin) is common.
Organ preservation -- keeping your body working the way it normally does -- is another research goal.
Sometimes when colorectal cancer recurs (comes back), it spreads to the peritoneum (the thin lining of the abdominal cavity and organs inside the abdomen). These cancers are often hard to treat.
Chemotherapy
Chemotherapy is an important part of treatment for many people with colorectal cancer, and doctors are constantly trying to make it more effective and safer.
Targeted therapy
Targeted therapy drugs work differently from standard chemotherapy drugs. They affect specific parts of cancer cells that make them different from normal cells. Several targeted therapy drugs are already used to treat advanced colorectal cancer. Researchers are studying the best way to produce these drugs and looking for new targeted therapy drugs. Studies are also looking at colorectal cancer cells to try to find specific gene changes (mutations) that might be targeted as part of treatment.
Studies are being done to see if using targeted therapy along with chemotherapy in earlier-stage cancers can help reduce the risk of recurrence.
Immunotherapy
An exciting area of research is the field of immunotherapy. This is treatment that uses the body’s own immune system to fight cancer.
Immune checkpoint inhibitors: An important part of the immune system is its ability to tell between normal cells in the body and those it sees as “foreign.” This lets the immune system attack the foreign cells while leaving the normal cells alone. To do this, it uses “checkpoint” proteins on certain immune cells. These proteins act like switches, needing to be turned on (or off) to start an immune response. Cancer cells sometimes use these checkpoints to keep from being attacked by the immune system.