This website uses cookies so that we can provide you with the best user experience possible. Cookie information is stored in your browser and performs functions such as recognising you when you return to our website and helping our team to understand which sections of the website you find most interesting and useful.
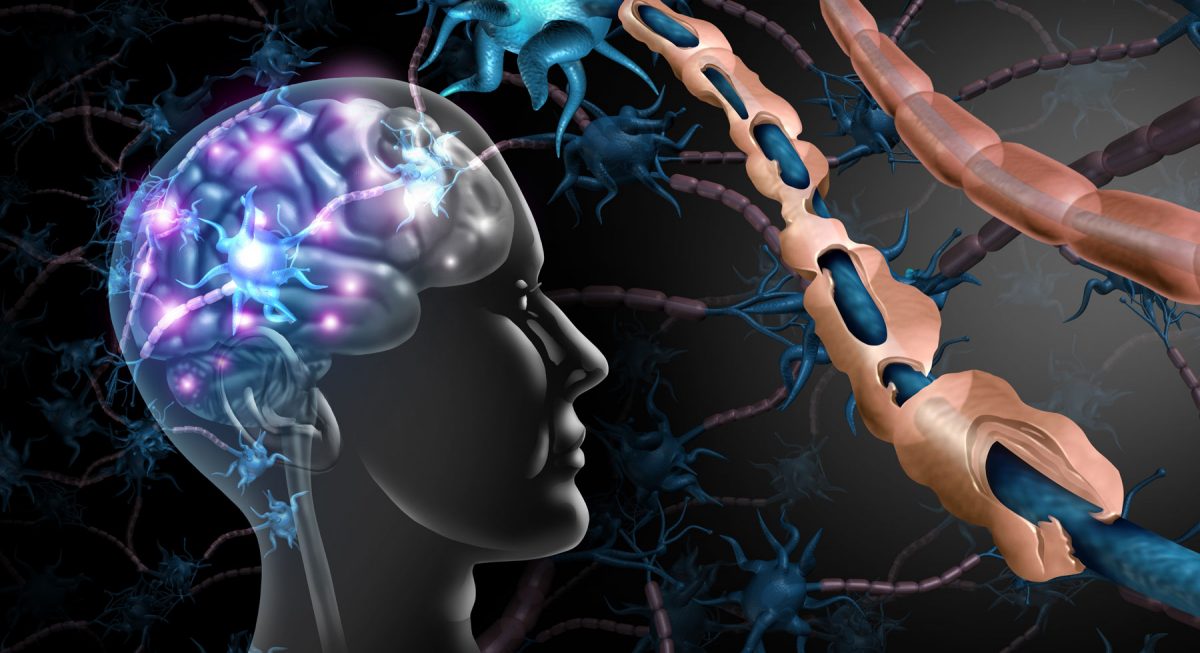
Multiple Sclerosis (MS) Disease
Multiple Sclerosis (MS) involves an immune-mediated process in which an abnormal response of the body’s immune system is directed against the central nervous system (CNS). The CNS is made up of the brain, spinal cord and optic nerves.
Within the CNS, the immune system causes inflammation that damages myelin — the fatty substance that surrounds and insulates the nerve fibers — as well as the nerve fibers themselves, and the specialized cells that make myelin.
- When myelin or nerve fibers are damaged or destroyed in MS, messages within the CNS are altered or stopped completely.
- Damage to areas of the CNS may produce a variety of neurological symptoms that will vary among people with MS in type and severity
- The damaged areas develop scar tissue which gives the disease its name – multiple areas of scarring or multiple sclerosis.
- The cause of MS is not known, but it is believed to involve genetic susceptibility, abnormalities in the immune system and environmental factors that combine to trigger the disease.
- People with MS typically experience one of four disease courses. There are over a dozen treatments to help modify the MS disease process.
Types of MS
Clinically Isolated Syndrome (CIS)
CIS is a first episode of neurologic symptoms caused by inflammation and demyelination in the central nervous system. The episode, which by definition must last for at least 24 hours, is characteristic of multiple sclerosis but does not yet meet the criteria for a diagnosis of MS because people who experience a CIS may or may not go on to develop MS.
When CIS is accompanied by lesions on a brain MRI (magnetic resonance imaging) that are similar to those seen in MS, the person has a high likelihood of a second episode of neurologic symptoms and diagnosis of relapsing-remitting MS. When CIS is not accompanied by MS-like lesions on a brain MRI, the person has a much lower likelihood of developing MS.
The 2017 diagnostic criteria for MS make it possible to diagnose MS in a person with CIS who also has specific findings on brain MRI that provide evidence of an earlier episode of damage in a different location and indicate active inflammation in a region other than the one causing the current symptoms. As MRI technology improves, the diagnosis of MS will be made more quickly and easily. In the meantime, individuals with CIS who are considered at high risk for developing MS may now be treated with a disease-modifying therapy that has been approved by the U.S. Food and Drug Administration (FDA) for that purpose. Early treatment of CIS has been shown to delay onset of MS.
Relapsing-Remitting MS (RRMS)
RRMS – the most common disease course – is characterized by clearly defined attacks of new or increasing neurologic symptoms. These attacks – also called relapses or exacerbations – are followed by periods of partial or complete recovery (remissions). During remissions, all symptoms may disappear, or some symptoms may continue and become permanent. However, there is no apparent progression of the disease during the periods of remission. At different points in time, RRMS can be further characterized as either active (with relapses and/or evidence of new MRI activity) or not active, as well as worsening (a confirmed increase in disability over a specified period of time following a relapse) or not worsening.
Approximately 85 percent of people with MS are initially diagnosed with RRMS.
Secondary Progressive MS (SPMS)
SPMS follows an initial relapsing-remitting course. Most people who are diagnosed with RRMS will eventually transition to a secondary progressive course in which there is a progressive worsening of neurologic function (accumulation of disability) over time. SPMS can be further characterized at different points in time as either active (with relapses and/or evidence of new MRI activity) or not active, as well as with progression (evidence of disease worsening on an objective measure of change over time, with or without relapses) or without progression.
Primary Progressive MS (PPMS)
PPMS is characterized by worsening neurologic function (accumulation of disability) from the onset of symptoms, without early relapses or remissions. PPMS can be further characterized at different points in time as either active (with an occasional relapse and/or evidence of new MRI activity) or not active, as well as with progression (evidence of disease worsening on an objective measure of change over time, with or without relapse or new MRI activity) or without progression.
Approximately 15 percent of people with MS are diagnosed with PPMS.
Treatments for MS
The available disease-modifying therapies used to treat MS are approved by the U.S. Food and Drug Administration (FDA) to treat “relapsing forms” of MS, which include RRMS as well as progressive MS in those individuals who continue to experience relapses. One of the medications has also been approved to treat PPMS. Scientists around the world are actively working to find more effective treatments for progressive forms of MS.