This website uses cookies so that we can provide you with the best user experience possible. Cookie information is stored in your browser and performs functions such as recognising you when you return to our website and helping our team to understand which sections of the website you find most interesting and useful.
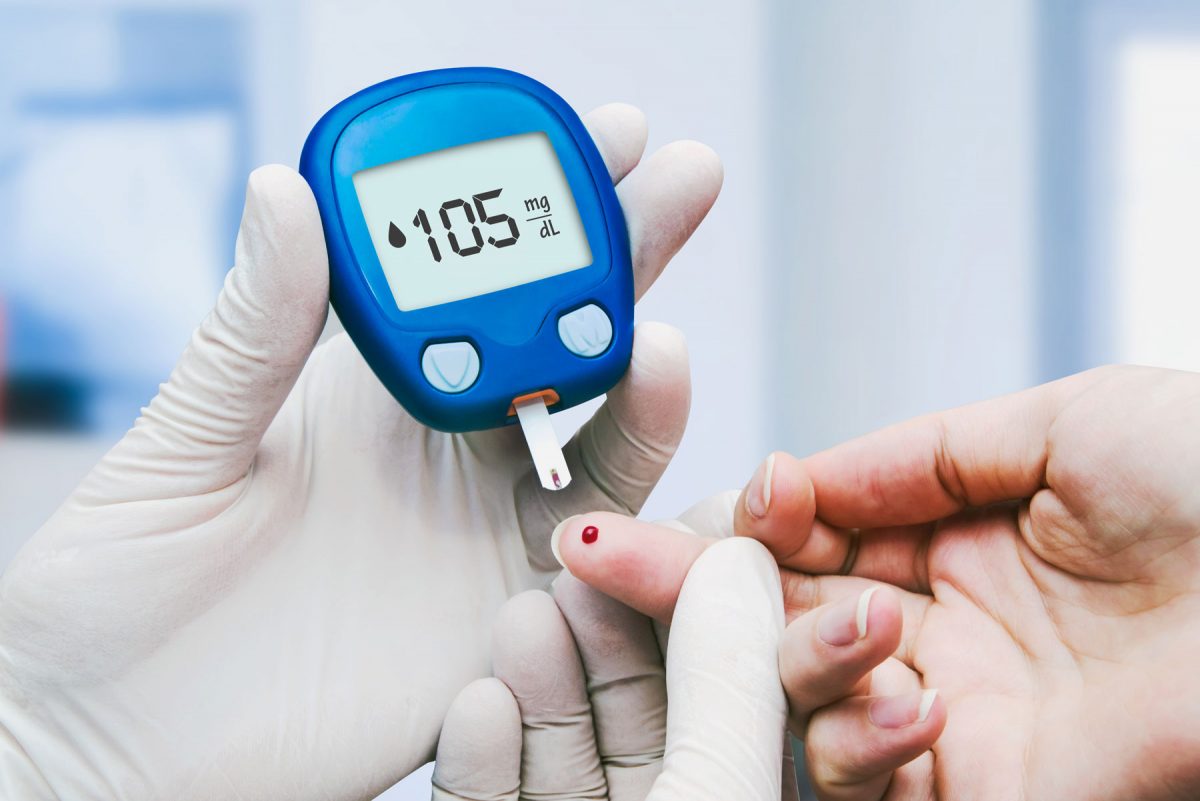
Diabetes Disease
Diabetes is a disease in which blood glucose, or blood sugar, levels are too high. Glucose comes from the foods. Insulin is a hormone that helps the glucose get into the cells to give them energy. With type 1 diabetes, the body does not make insulin. With type 2 diabetes, the more common type, the body does not make or use insulin well. Without enough insulin, the glucose stays in blood. A person can also have prediabetes. This means that the blood sugar is higher than normal but not high enough to be called diabetes. Having prediabetes puts the patient at a higher risk of getting type 2 diabetes.
Over time, having too much glucose in blood can cause serious problems. It can damage eyes, kidneys, and nerves. Diabetes can also cause heart disease, stroke and even the need to remove a limb. Pregnant women can also get diabetes, called gestational diabetes.
Blood tests can show if someone has diabetes. One type of test, the Hb A1C, can also check on how diabetes is being managed. Exercise, weight control and sticking to a meal plan can help control diabetes. Blood glucose levels should also be monitored and prescribed medicine must be taken regularly.
Diabetes Type 1 - Overview
Type 1 diabetes, once known as juvenile diabetes or insulin-dependent diabetes, is a chronic condition in which the pancreas produces little or no insulin. Insulin is a hormone needed to allow sugar (glucose) to enter cells to produce energy.
Different factors, including genetics and some viruses, may contribute to type 1 diabetes. Although type 1 diabetes usually appears during childhood or adolescence, it can develop in adults.
Despite active research, type 1 diabetes has no cure. Treatment focuses on managing blood sugar levels with insulin, diet and lifestyle to prevent complications.
Diabetes Type 2 Overview
Type 2 diabetes, once known as adult-onset or noninsulin-dependent diabetes, is a chronic condition that affects the way the body metabolizes sugar (glucose), body's important source of fuel.
With type 2 diabetes, the body either resists the effects of insulin — a hormone that regulates the movement of sugar into your cells — or doesn't produce enough insulin to maintain a normal glucose level.
More common in adults, type 2 diabetes increasingly affects children as childhood obesity increases. There's no cure for type 2 diabetes, the condition may be managed by eating well, exercising and maintaining a healthy weight. If diet and exercise aren't enough to manage blood sugar well, diabetes medications or insulin therapy may be necessary.
Symptoms
Signs and symptoms of type 2 diabetes often develop slowly. In fact, a person can have type 2 diabetes for years and not know it.
- Increased thirst and frequent urination
- Increased hunger
- Weight loss
- Fatigue
- Blurred vision
- Slow-healing sores or frequent infections
- Areas of darkened skin
Prevention
Healthy lifestyle choices can help prevent type 2 diabetes. Even if there is diabetes in one’s family, diet and exercise can help prevent the disease.
- Eat healthy foods
- Get physical
- Lose excess weight
Diagnosis
To diagnose type 2 diabetes, below tests are performed.
- Glycated hemoglobin (A1C) test
- Random blood sugar test
- Fasting blood sugar test: A blood sample will be taken after an overnight fast. A fasting blood sugar level less than 100 mg/dL (5.6 mmol/L) is normal. A fasting blood sugar level from 100 to 125 mg/dL (5.6 to 6.9 mmol/L) is considered prediabetes. If it's 126 mg/dL (7 mmol/L) or higher on two separate tests, the patients has diabetes.
- Oral glucose tolerance test: The American Diabetes Association recommends routine screening for type 2 diabetes beginning at age 45, especially if a person is overweight. If the results are normal, the test should be repeated every three years. If the results are borderline, the doctor indicates when to come back for another test.
Screening is also recommended for people who are under 45 and overweight if there are other heart disease or diabetes risk factors present, such as a sedentary lifestyle, a family history of type 2 diabetes, a personal history of gestational diabetes or blood pressure above 140/90 mm Hg.
If a person is diagnosed with diabetes, the doctor may do other tests to distinguish between type 1 and type 2 diabetes — since the two conditions often require different treatments.
Treatment
Management of type 2 diabetes includes:
- Healthy eating
- Regular exercise
- Possibly, diabetes medication or insulin therapy
- Blood sugar monitoring
These steps will help keep the blood sugar level closer to normal, which can delay or prevent complications.









